Entering the world of medical billing without understanding credentialing is like opening a clinic without a license; nothing moves forward, and revenue simply does not come in. Credentialing is not just paperwork; it is the foundation that allows healthcare providers to get paid, stay compliant, and build trust with both patients and insurance companies. Yet, many providers underestimate its impact until they face denied claims or delayed reimbursements.
If you are a provider, practice owner, or part of a billing team, understanding how credentialing works can directly influence your financial stability and operational efficiency. This article breaks down everything in a clear and structured way, helping you not only understand credentialing but also avoid costly mistakes and delays that most practices encounter.
What is Credentialing in Medical Billing?
Credentialing in medical billing is the process of verifying a healthcare provider’s qualifications so they can legally and professionally bill insurance companies for services. Without this approval, even the most accurate claims will be rejected because the provider is not recognized by the payer.
Think of credentialing as the gateway to revenue. Insurance companies need to confirm that a provider is licensed, trained, and authorized before allowing them into their network. Only after this process is complete can providers submit claims and receive reimbursements.
Here is what credentialing typically involves:
- Verification of education, training, and certifications
- Confirmation of active medical licenses
- Review of work history and professional background
- Validation of malpractice insurance coverage
- Cross-checking with national databases like CAQH
A simple example makes this clear. If a newly hired physician starts seeing patients before being credentialed, the clinic cannot bill insurance for those visits. This leads to immediate revenue loss.
Why Credentialing is Essential in Medical Billing
Credentialing is not just an administrative task; it directly affects whether a healthcare practice gets paid or not. Skipping or delaying this process can disrupt the entire revenue cycle.
When credentialing is handled properly, it creates a smooth path for claims to be accepted and processed quickly. When it is not, the result is denied claims, compliance risks, and financial setbacks.
Key reasons why credentialing matters:
- Ensures providers are eligible to bill insurance companies
- Reduces claim denials caused by provider ineligibility
- Supports compliance with healthcare regulations
- Builds credibility with both patients and payers
- Allows access to multiple insurance networks
From a financial perspective, the impact is significant:
- Uncredentialed providers can lose thousands in monthly revenue
- Delays in approval can push reimbursements back by 2 to 6 months
- Incorrect credentialing data can lead to repeated claim rejections
Many competitors mention the importance in general terms, but the real issue is cash flow. Without proper credentialing, even a busy practice can struggle financially because services cannot be converted into revenue.
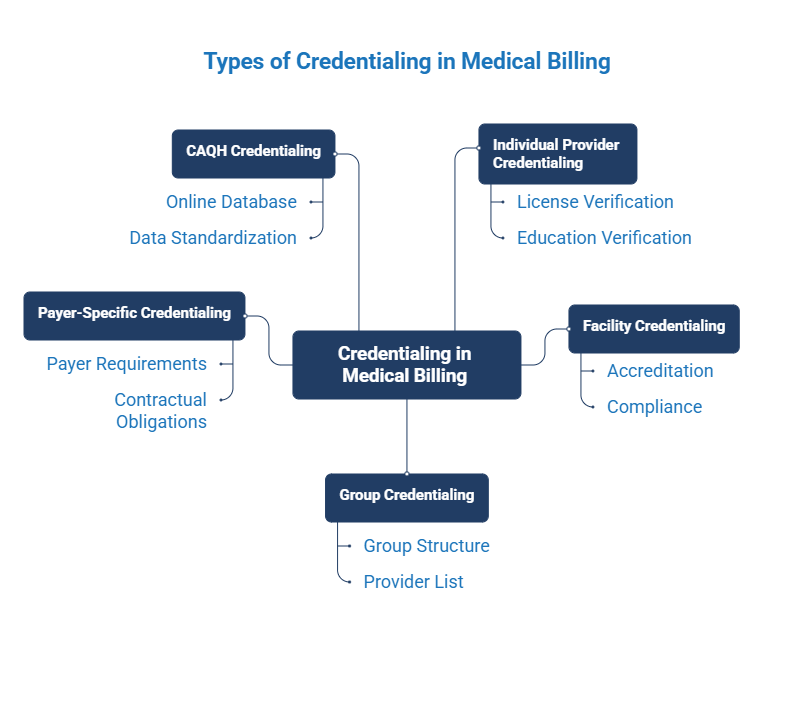
Types of Credentialing in Medical Billing
Credentialing is not a one-size process. It varies depending on the provider, facility, and payer requirements. Understanding these types helps practices manage approvals more efficiently and avoid confusion.
1. Individual Provider Credentialing
This applies to single healthcare professionals such as physicians, therapists, and nurses.
- Focuses on personal qualifications and licenses
- Required for independent practitioners
- Must be completed before joining insurance panels
2. Facility Credentialing
This is used for healthcare organizations rather than individuals.
- Applies to hospitals, clinics, and diagnostic centers
- Evaluates infrastructure, compliance, and services offered
- Required for facilities to bill insurance under their name
3. Group Credentialing
Group practices with multiple providers use this type of credentialing.
- Allows multiple providers to be linked under one organization
- Simplifies billing and administrative processes
- Still requires individual verification for each provider
4. Payer-Specific Credentialing
Each insurance company has its own requirements and approval process.
- Medicare and Medicaid follow government regulations
- Private insurers have unique application systems
- Approval timelines vary depending on the payer
5. CAQH Credentialing
CAQH acts as a centralized platform for provider data.
- Stores provider information in one place
- Reduces repetitive paperwork
- Requires regular updates and attestation
Types of Provider Credentialing
While general credentialing focuses on entities and systems, provider credentialing is more specific. It deals directly with the lifecycle of an individual provider’s approval status. Understanding these categories helps avoid lapses that can quietly disrupt billing.
Below are the main types every provider should be aware of:
Initial Credentialing
This is the first and most important step for any provider entering a network.
- Required when a provider joins a new practice or payer panel
- Involves full verification of credentials from scratch
- Typically takes the longest time, often 60 to 120 days
This stage sets the foundation. Any errors here can follow the provider for years.
Re-Credentialing (Revalidation)
Credentialing is not a one-time task. Providers must renew their status periodically.
- Usually required every 2 to 3 years
- Ensures licenses, certifications, and insurance are still valid
- Mandatory for maintaining participation with payers
Missing a re-credentialing deadline can lead to sudden claim denials, even for established providers.
Provisional Credentialing
In some cases, providers are allowed to work while their full credentialing is still under review.
- Temporary approval with limited permissions
- Often used in urgent hiring situations
- Comes with restrictions depending on payer policies
This can help maintain operations, but it is not a long-term solution.
Delegated Credentialing
This occurs when a third party handles credentialing on behalf of a payer.
- Common with large healthcare organizations
- Reduces administrative burden for providers
- Requires strict compliance and audits
It speeds up processes but requires strong internal systems to manage accuracy.
Credentialing Process in Medical Billing
Understanding the process step by step removes confusion and helps practices plan timelines more effectively. Credentialing is detailed and requires coordination between providers, billing teams, and insurance companies.
Here is how the process typically unfolds:
Step 1: Information Collection
The process begins with gathering all required provider details.
- Personal identification and contact information
- Medical education and training history
- State licenses and certifications
- Work history and references
Accuracy at this stage is critical because even small errors can cause delays later.
Step 2: Application Submission
Once data is compiled, applications are submitted to insurance payers.
- Each payer has its own forms and requirements
- Applications may be submitted manually or electronically
- Multiple submissions may be needed for different insurers
This step often requires careful tracking to ensure nothing is missed.
Step 3: Primary Source Verification
Insurance companies verify all submitted information directly from original sources.
- Medical boards confirm licenses
- Institutions verify education and training
- Databases check for sanctions or disciplinary actions
This is one of the most time-consuming parts of the process.
Step 4: CAQH Profile Setup and Attestation
Providers must maintain an updated CAQH profile.
- Acts as a centralized credentialing repository
- Information must be reviewed and attested regularly
- Many payers rely on CAQH for faster processing
Neglecting CAQH updates is a common reason for delays.
Step 5: Payer Review and Approval
After verification, the payer evaluates the application.
- Internal review committees assess eligibility
- Approval timelines can range from 60 to 180 days
- Additional documents may be requested
Patience and consistent follow-up are essential here.
Step 6: Contracting and Enrollment
Once approved, providers enter into agreements with payers.
- Fee schedules are defined
- Network participation is confirmed
- Billing permissions are established
This step directly impacts how much providers will be reimbursed.
Step 7: Activation for Billing
After everything is finalized, providers can begin billing.
- Claims can now be submitted and processed
- Payments can be received from insurance companies
- Revenue cycle officially becomes active
Skipping or rushing earlier steps often leads to issues at this stage.
Credentialing Process for Providers
From a provider’s perspective, credentialing can feel overwhelming, especially when balancing patient care with administrative demands. However, knowing what to expect makes the process much more manageable.
Instead of focusing only on steps, here is what providers actually experience:
What Providers Are Responsible For
Providers play a key role in ensuring the process moves smoothly.
- Submitting accurate and complete documentation
- Keeping licenses and certifications up to date
- Regularly reviewing and updating CAQH profiles
- Responding quickly to payer requests
Delays often happen when providers underestimate how much their input matters.
Essential Documents Checklist
Having documents ready in advance can significantly speed up credentialing.
- Active medical license
- DEA registration (if applicable)
- Malpractice insurance certificate
- National Provider Identifier (NPI)
- Board certifications
- Work history details
Keeping these organized reduces back-and-forth communication.
Common Delays Providers Face
Even well-prepared providers encounter challenges.
- Missing or outdated documents
- Inconsistent information across applications
- Slow responses from verification sources
- Payer-specific requirements causing confusion
These delays are not always avoidable, but they can be minimized.
How Providers Can Speed Up Credentialing?
Small actions can make a big difference in timelines.
- Double-check all submitted information for accuracy
- Maintain an updated CAQH profile at all times
- Track application status proactively
- Work with experienced credentialing specialists
A proactive approach can cut weeks, sometimes months, off the process.
Importance of Medical Credentialing for Providers
Credentialing is not just about approval; it directly determines whether a provider can operate smoothly, earn revenue, and maintain credibility. Its impact goes far beyond paperwork and touches every part of a healthcare practice.
Here is why it plays such a critical role:
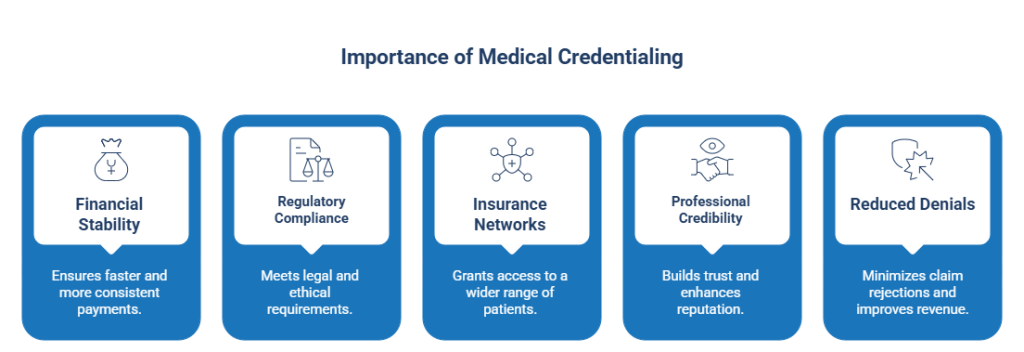
Financial Stability and Faster Payments
Without credentialing, providers simply cannot bill insurance companies.
- Ensures claims are accepted instead of rejected
- Reduces delays in reimbursement cycles
- Supports consistent cash flow for the practice
Even a short delay in credentialing can result in significant revenue loss.
Regulatory Compliance
Healthcare is heavily regulated, and credentialing helps providers stay within legal boundaries.
- Confirms providers meet licensing requirements
- Protects against penalties and legal issues
- Aligns with payer and government standards
Non-compliance can lead to audits, fines, or even loss of practice rights.
Access to Insurance Networks
Credentialing opens the door to a larger patient base.
- Allows providers to join multiple payer networks
- Increases patient accessibility and volume
- Enhances practice growth opportunities
Without it, providers are limited to self-pay patients, which restricts growth.
Trust and Professional Credibility
Patients and payers both rely on credentialing as a mark of quality.
- Builds confidence in provider qualifications
- Strengthens relationships with insurance companies
- Improves the overall reputation of the practice
Trust plays a huge role in patient retention and referrals.
Reduction in Claim Denials
Proper credentialing ensures smoother billing operations.
- Eliminates eligibility-related claim rejections
- Improves claim acceptance rates
- Reduces administrative rework
This directly saves time, effort, and operational costs.
Common Challenges in Medical Credentialing
Despite its importance, credentialing is often one of the most frustrating processes for providers and billing teams. It requires patience, accuracy, and constant follow-up.
Here are the most common challenges faced in real-world scenarios:
- Lengthy approval timelines
- Some payers take 3 to 6 months for approval
- Delays can disrupt revenue planning
- Incomplete or incorrect documentation
- Missing details can restart the entire process
- Even minor inconsistencies cause rejection
- Payer-specific requirements
- Each insurer has different forms and criteria
- Managing multiple applications becomes complex
- Lack of proper tracking systems
- Applications get lost or delayed without follow-ups
- No visibility into approval status
- Re-credentialing lapses
- Expired credentials can lead to sudden claim denials
- Many practices overlook renewal timelines
What most discussions miss is the cost of these challenges. Every delay translates into lost revenue, increased administrative workload, and unnecessary stress for providers.
How Long Does Credentialing Take?
One of the most common questions providers ask is about timelines. The answer varies, but understanding the general range helps set realistic expectations.
Typical Timeframes
- Medicare: 60 to 90 days
- Medicaid: 90 to 120 days
- Private insurers: 60 to 180 days
Factors That Affect Timeline
Several variables can speed up or slow down the process:
- Accuracy of submitted information
- Responsiveness of the provider
- Verification delays from institutions
- Payer workload and internal processes
Ways to Reduce Delays
- Submit complete and verified documents from the start
- Keep CAQH information updated and attested
- Follow up regularly with payers
- Use experienced credentialing support
Being proactive is the difference between a 2-month process and a 6-month delay.
Credentialing vs Enrollment vs Privileging
These terms are often used interchangeably, but they serve very different purposes. Understanding the distinction helps avoid confusion and operational mistakes.
| Aspect | Credentialing | Enrollment | Privileging |
| Purpose | Verifies provider qualifications | Registers provider with payer | Grants clinical permissions |
| Focus | Education, licenses, experience | Insurance network participation | Scope of medical procedures |
| Outcome | Provider is approved | Provider can bill insurance | Provider can perform specific services |
In simple terms, credentialing confirms who you are, enrollment allows you to get paid, and privileging determines what you are allowed to do clinically.
Best Practices for Smooth Credentialing
A well-managed credentialing system can save time, reduce stress, and improve revenue flow. The difference between smooth and chaotic processes often comes down to a few key habits.
Here are proven best practices:
- Keep all provider documents organized and updated
- Maintain an active and accurate CAQH profile
- Track application status with a dedicated system
- Set reminders for license and certification renewals
- Communicate consistently with payers
- Standardize internal processes for efficiency
Small improvements in organization can lead to major gains in turnaround time.
Should You Outsource Credentialing Services?
Many practices struggle to decide whether to handle credentialing in-house or outsource it. The right choice depends on resources, expertise, and workload.
Benefits of Outsourcing
- Reduces administrative burden
- Speeds up application processing
- Improves accuracy and compliance
- Allows providers to focus on patient care
Potential Drawbacks
- Additional cost
- Dependence on external teams
- Requires choosing a reliable partner
When Outsourcing Makes Sense
- Rapidly growing practices
- Limited administrative staff
- Frequent credentialing and re-credentialing needs
For many providers, outsourcing to a reliable credentialing company is not just a convenience; it becomes a strategic decision to protect revenue and efficiency.
The Bottom Line
Credentialing in medical billing is not just a formality; it is the backbone of a provider’s ability to generate revenue and operate smoothly. From verifying qualifications to enabling insurance reimbursements, every step plays a critical role in the healthcare ecosystem.
Providers who understand and manage credentialing effectively experience fewer claim denials, faster payments, and stronger growth opportunities. On the other hand, neglecting it can lead to delays, compliance issues, and financial loss.
Taking a proactive and structured approach to credentialing is not optional; it is essential for long-term success in today’s healthcare environment.





