In the world of medical billing, even a small coding mistake can delay payments and disrupt your entire revenue cycle. One of the most common yet often misunderstood issues is the CO-4 denial code, a rejection that signals a mismatch or missing modifier in your claim. If left unresolved, it can lead to repeated denials, lost revenue, and unnecessary administrative burden.
The good news? CO-4 denials are highly preventable when you understand their root cause and apply the right corrective actions. In this comprehensive guide, you’ll learn exactly what CO-4 means, why it happens, how Medicare handles it, and most importantly, the proven steps to fix and prevent it, so you can submit cleaner claims and get paid faster.
What is CO-4 Denial Code?
The CO-4 denial code is a claim adjustment reason code used by insurance payers to indicate that a submitted procedure code is inconsistent with the modifier used, or a required modifier is missing. In simpler terms, it means the claim was rejected because the modifier attached to the CPT or HCPCS code is either incorrect, incomplete, or not supported by the procedure billed.
Modifiers play a critical role in medical billing; they provide additional information about a service, such as whether it was altered, performed multiple times, or done under specific circumstances. When modifiers are missing or incorrectly applied, payers cannot accurately interpret the claim, leading to denial under CO-4.
This denial typically falls under a contractual obligation (CO) category, meaning the provider is responsible for correcting the error before resubmitting the claim. Understanding this code is essential for billing teams, as repeated CO-4 denials can significantly slow down reimbursements and increase administrative workload.
CO-4 Denial Code Reason
The root causes behind denial CO-4 are the first step toward reducing claim rejections and improving clean claim rates. Most CO-4 denials occur due to issues related to improper modifier usage or lack of proper documentation.
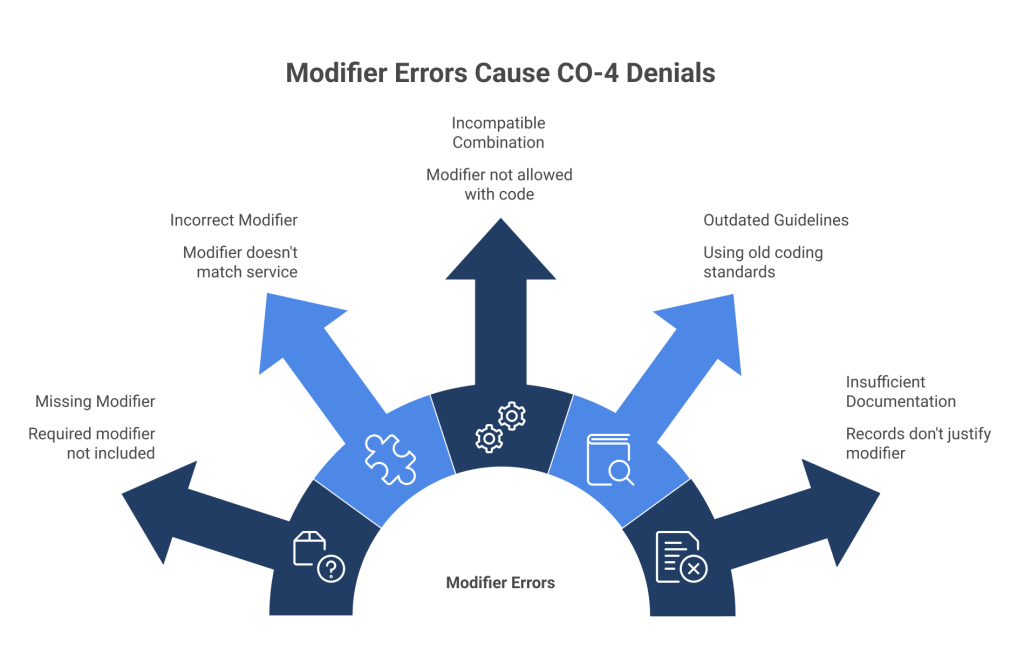
Missing Modifier: A required modifier was not included with the procedure code, making the claim incomplete.
Incorrect Modifier Usage: The modifier used does not match the service performed or is not appropriate for the CPT code billed.
Incompatible CPT Code and Modifier Combination: Some modifiers cannot be used with certain procedure codes, leading to automatic rejection.
Outdated Coding Guidelines: Using old or incorrect coding standards can result in invalid modifier combinations.
Insufficient Documentation: The medical records do not justify the use of the modifier, causing the payer to deny the claim.
Real-Life Examples
- A provider bills a surgical procedure but forgets to include modifier -59 for a distinct procedural service, resulting in a CO-4 denial.
- A claim includes modifier -25 for an evaluation and management (E/M) service, but documentation does not support a separately identifiable service.
- A billing team applies a modifier that is not recognized by the payer for that specific CPT code.
These examples highlight how even minor errors in modifier usage can lead to claim denials. Identifying these issues early can save time, reduce rework, and improve overall billing efficiency.
Medicare Denial Code CO-4
When it comes to Medicare denial code CO-4, the rules become even more stringent. Medicare, governed by the Centers for Medicare & Medicaid Services (CMS), strictly enforces correct modifier usage to ensure accurate billing and compliance.
Under Medicare guidelines, a CO-4 denial typically means:
- A required modifier is missing
- The modifier used is not appropriate for the billed service
- The modifier does not align with Medicare’s coding policies
Key Medicare-Specific Considerations
- Strict Modifier Validation
Medicare systems automatically check whether modifiers are valid for specific CPT/HCPCS codes. Any mismatch triggers a CO-4 denial. - National Correct Coding Initiative (NCCI) Edits
Medicare applies National Correct Coding Initiative edits to prevent improper coding combinations. If a modifier doesn’t correctly override an edit, the claim is denied. - Documentation Requirements
Medicare requires clear and detailed documentation to justify modifier usage. Without proper support, even correctly applied modifiers may be denied. - Limited Flexibility Compared to Commercial Payers
Unlike some private insurers, Medicare rarely allows leniency for incorrect modifiers, making first-pass accuracy critical.
Medicare vs. Commercial Payers
While commercial insurers may sometimes provide flexibility or allow easier corrections, Medicare follows standardized national rules. This makes it essential for billing teams to stay updated with CMS guidelines and ensure claims are compliant before submission.
Commonly Used Remark Codes for CO-4 Denial
Remark codes, also known as Remittance Advice Remark Codes (RARC), provide additional details explaining why a claim was denied under CO-4. These codes help billing teams pinpoint the exact issue and take corrective action quickly.
Frequently Seen Remark Codes
- M76: Missing, incomplete, or invalid modifier
- N290: Missing, incomplete, or invalid rendering provider primary identifier
- N297: Missing, incomplete, or invalid modifier(s)
How to Interpret These Codes
Remark codes act as supporting explanations for the denial:
- They clarify whether the issue is a missing modifier or an incorrect one
- They guide billing teams on what needs to be corrected before resubmission
- They reduce guesswork, allowing faster claim resolution
For example, if a claim is denied with CO-4 and remark code M76, it clearly indicates that the modifier is either missing or invalid, prompting the biller to review and correct modifier usage immediately.
CO-4 Denial Code Solution (Step-by-Step)
Fixing a CO-4 denial code isn’t complicated, but it does require a structured, detail-oriented approach. The key is to quickly identify the issue, correct it accurately, and resubmit a clean claim to avoid further delays.
Step 1: Identify the Error
Start by reviewing the denial details carefully:
- Check the CPT/HCPCS code billed
- Review the modifier used (or missing)
- Look at accompanying remark codes (e.g., M76, N297)
This step helps you pinpoint whether the issue is a missing modifier, an incorrect modifier, or an invalid combination.
Step 2: Verify Documentation
Before making any corrections:
- Cross-check clinical notes and provider documentation
- Ensure the modifier is medically necessary and properly supported
- Confirm that the service justifies the modifier used
If documentation does not support the modifier, you may need to consult the provider before resubmitting.
Step 3: Correct the Claim
Now apply the appropriate fix:
- Add the correct modifier (if missing)
- Replace incorrect modifiers with valid ones
- Remove modifiers that are not required
- Ensure compliance with payer-specific and CMS guidelines
Accuracy at this stage is critical to avoid repeat denials.
Step 4: Resubmit the Claim
Once corrected:
- Resubmit within the payer’s timely filing limit
- Mark the claim as corrected (if required)
- Double-check all fields before submission
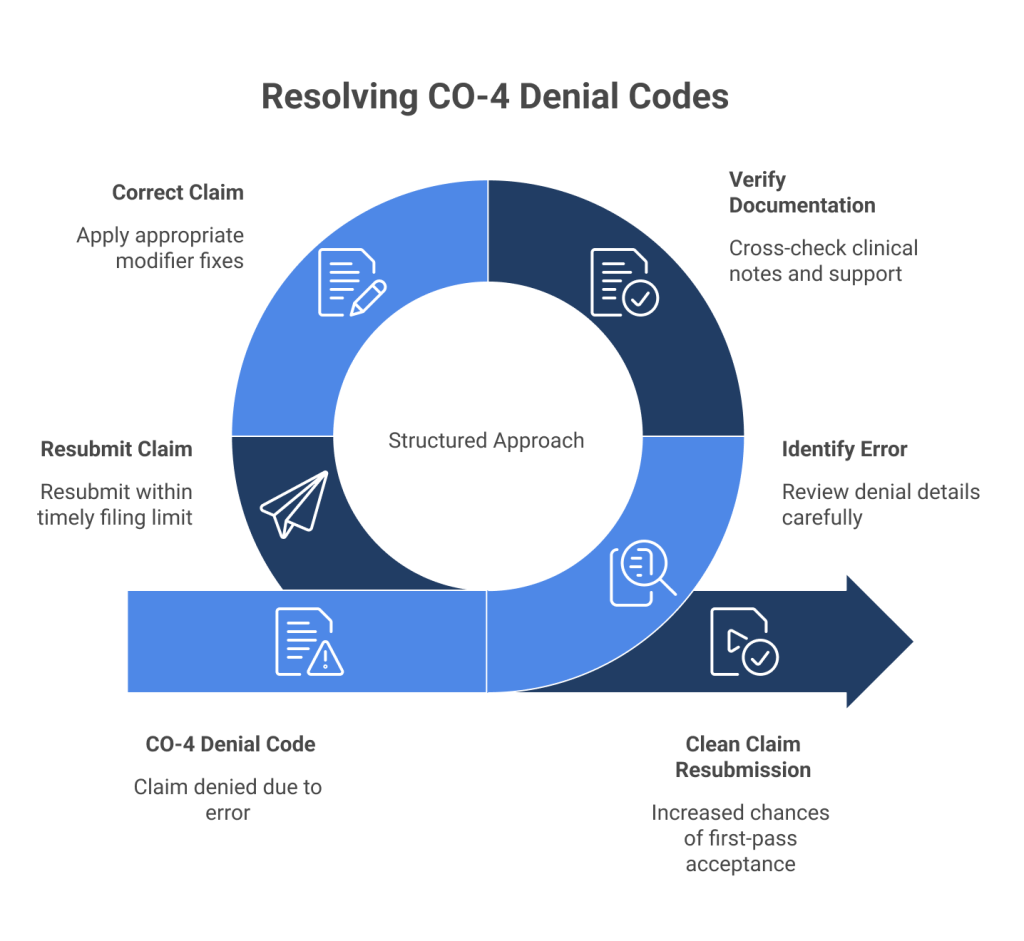
A clean, error-free resubmission increases the chances of first-pass acceptance.
How to Prevent CO-4 Denials?
Prevention is always more efficient than correction. By implementing the right processes, you can significantly reduce denial CO-4 occurrences and improve your revenue cycle performance.
- Use Updated Coding Resources: Always follow the latest CPT, HCPCS, and payer-specific guidelines.
- Invest in Staff Training: Regular training ensures coders and billers understand proper modifier usage.
- Implement Claim Scrubbing Tools: Automated systems can detect missing or invalid modifiers before submission.
- Conduct Regular Audits: Internal audits help identify recurring errors and improve accuracy over time.
- Standardize Workflow Processes: Create clear SOPs for coding and billing to minimize inconsistencies.
Best Practices for Medical Billing Teams
To consistently reduce CO-4 denials and boost reimbursement rates, medical billing teams should adopt a proactive and quality-focused approach:
- Pre-Submission Quality Checks: Review claims thoroughly before submission to catch modifier-related errors early.
- Clear Communication with Providers: Ensure providers document services accurately to support modifier usage.
- Stay Updated with Industry Changes: Keep track of updates from the Centers for Medicare & Medicaid Services and other payers.
- Leverage Technology: Use advanced billing software to automate validation and reduce manual errors.
- Track Denial Trends: Analyze denial reports regularly to identify patterns and implement corrective actions.
Conclusion
The CO-4 denial code is one of the most common yet avoidable challenges in medical billing. It primarily stems from incorrect or missing modifiers, an issue that can disrupt cash flow and increase administrative workload if not addressed properly. By understanding the CO-4 denial code reason, applying the right solutions, and staying compliant with Medicare guidelines, billing teams can significantly reduce denial rates.
The key takeaway is simple: accuracy in modifier usage is critical. With proper training, updated coding practices, and proactive denial management, healthcare organizations can submit cleaner claims, accelerate reimbursements, and maintain a more efficient revenue cycle.Struggling with frequent claim denials or looking to improve your billing efficiency? Partner with experienced medical billing professionals from ORCM and take control of your revenue cycle, reduce denials, increase approvals, and get paid faster.





