If you’ve ever looked at a medical bill and wondered why some charges simply disappear, you’re not alone. One of the most misunderstood concepts in healthcare finance is the write-off in medical billing, and it plays a critical role in how providers get paid and how much patients actually owe.
In simple terms, a write-off is the portion of a medical bill that a healthcare provider agrees not to collect. But here’s where it gets interesting: not all write-offs are the same. Some are required by insurance contracts, others happen because patients can’t pay, and some occur due to billing errors or administrative decisions.
Exploring how write-offs work isn’t just important for billing professionals; it’s essential for providers trying to protect revenue and for patients who want clarity about their financial responsibility.
How Write-Offs Work in Medical Billing?
To fully understand write-offs, it’s important to see where they fit into the medical billing process. A write-off doesn’t happen randomly; it occurs after a claim has been processed by the insurance company and the final payable amount has been determined.
When a patient receives medical care, the provider first generates a bill based on their standard charges. This bill is then submitted to the patient’s insurance company. Once the insurer reviews (or “adjudicates”) the claim, they decide how much of the billed amount is actually allowed under the patient’s plan.
This is where the concept of a write-off comes into play.
Let’s say a provider charges $1,000 for a procedure. However, the insurance company has a negotiated agreement that only allows $700 for that same service. The remaining $300 is not simply ignored; it is officially recorded as a write-off, meaning the provider agrees not to collect that portion.
Out of the allowed $700, the insurance may pay a portion (for example, $500), while the rest ($200) becomes the patient’s responsibility in the form of copay, coinsurance, or deductible. Importantly, the written-off $300 is not billable to the patient.
This process highlights a key reality in healthcare: the amount providers charge is often different from what they actually receive. Write-offs help bridge that gap and ensure billing aligns with contractual agreements.
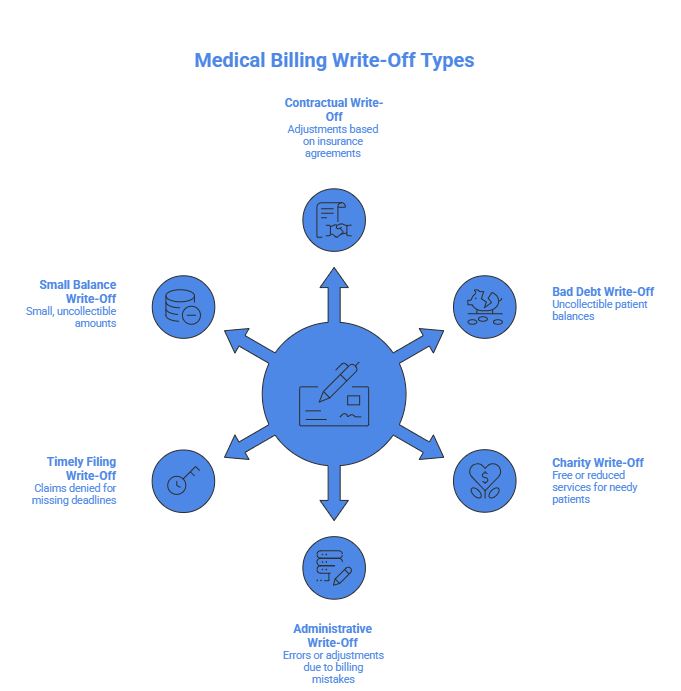
Types of Write-Offs in Medical Billing
Write-offs in medical billing are not all created for the same reason. In fact, they can occur due to contractual obligations, financial hardship, operational inefficiencies, or even simple administrative decisions. Understanding these types is essential because each one affects revenue differently and requires a different management approach.
1. Contractual Write-Off
The most common and important type is the contractual write-off. This occurs when a healthcare provider has a pre-negotiated agreement with an insurance company to accept a reduced rate for services.
For example, if a provider’s standard charge for a service is higher than what the insurer has agreed to pay, the difference must be written off. This is not optional; it is legally binding under the contract between the provider and the payer.
One important point that often confuses patients is that this amount cannot be transferred to them. In other words, if a charge is contractually written off, the provider cannot bill the patient for it. The provider absorbs this cost as part of doing business with that insurance company.
2. Bad Debt Write-Off
A bad debt write-off happens when a patient is responsible for a portion of the bill but fails to pay despite multiple collection efforts.
Unlike contractual write-offs, this type represents an actual financial loss for the provider. After a certain period, once all reasonable attempts to collect the payment have been exhausted, the unpaid balance is written off as bad debt.
This type of write-off is particularly significant because it reflects issues like:
- Patient affordability challenges
- Ineffective collection processes
- Lack of financial counseling upfront
For providers, high bad debt write-offs can signal deeper problems in revenue cycle management.
3. Charity or Financial Hardship Write-Off
In some cases, providers intentionally write off bills to support patients who are unable to afford care. This is known as a charity care write-off or financial hardship write-off.
Healthcare organizations often have formal policies in place to determine eligibility for such programs. Patients who meet certain income or financial criteria may have part or all of their bills forgiven.
While this results in reduced revenue, it also plays an important role in:
- Improving access to healthcare
- Supporting community health
- Maintaining a positive patient-provider relationship
4. Administrative Write-Off
Administrative write-offs occur due to internal issues within the billing process. These might include coding errors, duplicate charges, or system-related mistakes that make it impractical or impossible to collect the billed amount.
Although these write-offs may seem minor, they can add up over time and indicate inefficiencies in billing operations. Frequent administrative write-offs often point to the need for better staff training, improved systems, or stronger quality checks.
5. Timely Filing Write-Off
A timely filing write-off happens when a claim is not submitted within the insurance company’s required timeframe. Every payer has strict deadlines, and missing them can result in claim denial.
When this happens, the provider may have no choice but to write off the entire amount, especially if the delay was their responsibility. This type of write-off is particularly avoidable and often reflects workflow or process gaps.
6. Small Balance Write-Off
In some situations, the cost of collecting a small outstanding balance is higher than the amount itself. In these cases, providers may choose to write off the remaining balance rather than pursue collection.
This is known as a small balance write-off, and it is typically used as a practical decision to save time and administrative effort.
What is Contractual Write-Off in Medical Billing?
Among all types of write-offs, the contractual write-off is the most common and arguably the most important to understand.
A contractual write-off occurs when a healthcare provider agrees, through a contract with an insurance company, to accept a reduced payment for services. This agreement is established before any treatment is provided, which means the provider already knows they will not receive the full billed amount.
For example, a provider might charge $1,000 for a procedure, but the insurance company has negotiated an allowed amount of $700. The remaining $300 is not considered collectible; it is automatically written off as a contractual adjustment.
What makes this type of write-off unique is that it is mandatory and legally binding. Providers who are in-network with an insurance company must comply with these agreed rates. They cannot bill the patient for the difference, even if their original charge was higher.
This is a key point that often causes confusion. Many patients assume that anything not paid by insurance becomes their responsibility. However, in the case of contractual write-offs, that is not true. The provider absorbs this difference entirely.
From a business perspective, contractual write-offs are not necessarily “losses” in the traditional sense. Instead, they represent the trade-off providers accept in exchange for:
- Access to a larger patient base
- Faster and more predictable payments
- Established relationships with insurers
In short, contractual write-offs are built into the financial structure of modern healthcare and are a standard part of revenue cycle management.
Who is Responsible for Paying the Write-Off Amount?
This is one of the most frequently asked and most misunderstood questions in medical billing.
The simple answer is: no one pays the write-off amount.
When a charge is written off, it means the provider has decided (or is contractually obligated) not to collect that portion of the bill. It is removed from accounts receivable and no longer considered payable by any party.
However, to fully understand this, it’s important to distinguish between three different components of a medical bill:
First, there is the insurance payment, which is the portion covered by the patient’s health plan.
Second, there is the patient’s responsibility, which includes deductibles, copays, and coinsurance. This is the amount the patient is legally required to pay.
Finally, there is the write-off, which is neither billed to insurance nor to the patient. It simply disappears from the balance because it is not collectible.
Can Doctors Write Off Unpaid Bills?
Yes, doctors can write off unpaid bills, but only under specific circumstances, and often with strict guidelines.
In practice, providers write off unpaid balances in situations where collecting the payment is either not possible or not practical. One common example is bad debt, where a patient is responsible for a portion of the bill but fails to pay despite repeated reminders and collection efforts. After a certain period, the provider may classify the balance as uncollectible and write it off.
Another situation involves charity care or financial hardship. If a patient demonstrates an inability to pay due to financial constraints, the provider may choose to forgive part or all of the bill. Many healthcare organizations have formal policies to evaluate and approve such cases.
However, it’s important to understand that write-offs are not something providers can apply freely without consideration. There are several factors they must take into account, including:
- Insurance contracts: Providers cannot arbitrarily waive patient responsibilities like copays or deductibles if it violates their agreement with insurers.
- Legal and compliance requirements: Improper or undocumented write-offs can raise red flags during audits and may be considered fraudulent in certain cases.
- Internal policies: Most organizations have structured processes for approving and documenting write-offs to ensure transparency and accountability.
In other words, while doctors do have the ability to write off unpaid bills, it must be done carefully, ethically, and in compliance with both contractual and regulatory standards.
What is Bad Debt Write-Off in Medical Billing?
A bad debt write-off in medical billing occurs when a patient is responsible for paying a portion of their bill but fails to do so, even after multiple collection attempts. At this point, the provider determines that the amount is unlikely to be recovered and removes it from their accounts receivable.
Unlike contractual write-offs, which are expected and agreed upon, bad debt represents a true financial loss for the provider.
This situation typically arises after the insurance company has already paid its share, and the remaining balance has been assigned to the patient. The provider may then go through a series of steps, such as sending statements, making follow-up calls, or even involving a collection agency. If all efforts fail, the unpaid amount is written off as bad debt.
Bad debt write-offs are often influenced by several factors, including:
- High patient deductibles and out-of-pocket costs
- Lack of upfront financial communication
- Inefficient billing or follow-up processes
For healthcare providers, a high rate of bad debt write-offs can signal deeper issues in the revenue cycle, such as poor patient engagement or ineffective collection strategies.
From a patient perspective, it’s important to note that even though the provider writes off the debt internally, it may still impact the patient if the account was sent to collections before being written off.
Write-Off vs Adjustment in Medical Billing
One of the most common areas of confusion in medical billing is the difference between a write-off and an adjustment. While both involve changes to a bill, they serve very different purposes and have different financial implications.
Here’s a clear comparison to help you understand:
| Feature | Write-Off | Adjustment |
| Definition | An amount that is no longer collectible and has been removed from accounts receivable | A correction made to a billing error or claim discrepancy |
| Financial Impact | Represents an actual revenue loss for the provider | Does not always result in a financial loss |
| Reason | Contractual agreements, bad debt, charity care, or uncollectible balances | Coding errors, duplicate charges, or claim corrections |
| Patient Responsibility | Not billable to the patient (in most cases) | May change patient responsibility depending on the correction |
| Reversibility | Typically, final and cannot be reversed | Can sometimes be corrected or reversed |
| Common Example | Difference between billed and allowed amount | Fixing an incorrect CPT code |
In simple terms, a write-off means the provider accepts that the money will not be collected, while an adjustment is simply a correction to ensure billing accuracy.
Impact of Write-Offs on Healthcare Providers
Write-offs are not just accounting entries; they have a direct and often significant impact on a healthcare provider’s financial health.
At a basic level, every write-off reduces the total revenue a provider can collect. While some write-offs, like contractual ones, are expected and built into pricing strategies, others, such as bad debt or administrative write-offs, can negatively affect profitability.
One of the most immediate impacts is on cash flow. When large portions of billed charges are written off, the actual cash coming into the organization is lower than anticipated. Over time, this can create financial strain, especially for smaller practices with limited margins.
Write-offs also influence key performance indicators (KPIs) in revenue cycle management, such as:
- Net collection rate
- Accounts receivable (AR) days
- Denial rates
A high volume of avoidable write-offs, like those caused by billing errors or missed deadlines, often indicates inefficiencies in internal processes. This can lead to lost revenue opportunities and increased operational costs.
However, not all impacts are negative. Strategic write-offs, such as charity care, can enhance a provider’s reputation, improve patient satisfaction, and support long-term community trust.
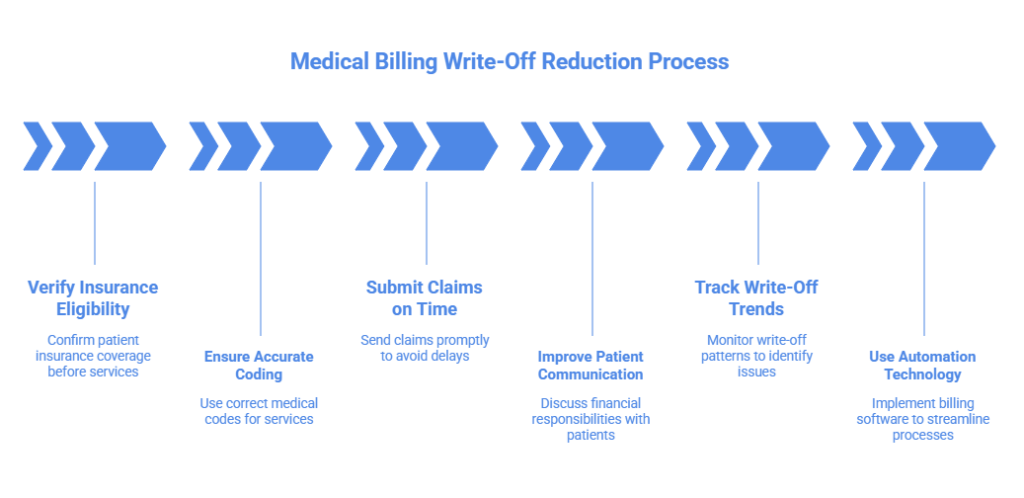
How to Reduce Write-Offs in Medical Billing?
Reducing write-offs is one of the most effective ways to improve revenue without increasing patient volume. While some write-offs, like contractual ones, are unavoidable, many others result from preventable errors, inefficiencies, or poor communication. By strengthening processes across the revenue cycle, healthcare providers can significantly minimize unnecessary financial losses.
Verify Insurance Eligibility in Advance: Always confirm patient coverage, benefits, and authorization requirements before providing services. This helps prevent claim denials and unexpected write-offs later.
Ensure Accurate Medical Coding and Documentation: Coding errors are one of the leading causes of denied claims. Proper documentation and certified coders reduce the risk of rejections that may eventually lead to write-offs.
Submit Claims on Time: Missing payer deadlines can result in complete claim denials. Implementing strict timelines and automated tracking ensures claims are submitted within the allowed timeframe.
Improve Patient Financial Communication: Clearly explain costs, insurance coverage, and patient responsibility upfront. This reduces confusion and lowers the chances of unpaid balances becoming bad debt.
Track and Analyze Write-Off Trends: Regularly review write-off reports to identify patterns. Understanding whether losses come from denials, errors, or patient non-payment helps in taking corrective actions.
Use Automation and Billing Technology: Modern billing systems reduce manual errors, improve claim accuracy, and streamline follow-ups, leading to fewer avoidable write-offs.
Best Practices for Managing Write-Offs
Managing write-offs effectively is just as important as reducing them. A structured approach ensures that write-offs are properly tracked, justified, and minimized over time.
Establish Clear Write-Off Policies
Define when and how write-offs should be applied. This ensures consistency and prevents unauthorized or unnecessary adjustments.
Categorize Write-Offs Correctly
Separate contractual, bad debt, administrative, and charity write-offs. Proper categorization helps in accurate financial reporting and analysis.
Conduct Regular Audits
Periodic reviews of billing and write-offs help identify errors, compliance risks, and revenue leakage.
Monitor Key Performance Indicators (KPIs)
Track metrics like net collection rate, AR days, and write-off ratios to evaluate financial health and operational efficiency.
Train Billing and Administrative Staff
Well-trained staff are less likely to make errors that lead to write-offs. Continuous education improves overall billing accuracy.
Maintain Proper Documentation
Every write-off should be supported with clear documentation to ensure transparency and compliance during audits.
Legal & Compliance Considerations
Write-offs in medical billing are not just financial decisions; they are also subject to strict legal and regulatory guidelines. Improper handling of write-offs can lead to compliance issues, audits, and even penalties.
Healthcare providers must ensure that all write-offs are applied in accordance with insurance contracts and applicable laws. For example, routinely waiving patient responsibilities such as copays or deductibles without valid reasons may violate payer agreements and could be considered fraudulent.
Proper documentation is essential. Every write-off, whether contractual, bad debt, or charity, should be clearly recorded with a valid reason and supporting evidence. This helps demonstrate transparency and accountability during audits.
Additionally, providers should have internal controls in place to prevent misuse or overuse of write-offs. Regular monitoring and compliance checks can reduce the risk of legal complications and ensure that billing practices remain ethical and aligned with industry standards.
Real-Life Examples of Write-Offs
A contractual write-off occurs when a provider charges $800 for a service, but the insurance company allows only $600. The $200 difference is written off due to the contract, and the patient is not responsible for it.
A bad debt write-off might happen when a patient owes $150 after insurance payment but fails to pay despite multiple reminders. After exhausting collection efforts, the provider writes off the amount as uncollectible.
A charity write-off can occur when a patient qualifies for financial assistance due to low income. In such cases, the provider may forgive the entire outstanding balance to support the patient.
These examples highlight how write-offs can arise from different situations, each with its own financial and operational implications.
Conclusion
Write-offs in medical billing are a fundamental part of the healthcare revenue cycle, but they are often misunderstood. From contractual obligations to bad debt and charity care, each type of write-off serves a different purpose and impacts providers in different ways.
For healthcare organizations, the key is not just understanding write-offs but managing them strategically. By improving billing processes, ensuring compliance, and enhancing patient communication, providers can reduce unnecessary losses and maintain financial stability.
For patients, understanding write-offs brings clarity and peace of mind, helping them better navigate medical bills and know exactly what they are (and are not) responsible for.
In the end, effective write-off management is not just about numbers; it’s about creating a more transparent, efficient, and patient-friendly healthcare system.





