What if the biggest reason behind your claim denials isn’t coding, but documentation? In a billing environment, even highly skilled coders can’t compensate for incomplete or unclear clinical records. That’s exactly why CDI in healthcare has become a critical driver of both financial performance and compliance.
It ensures that every diagnosis, procedure, and patient condition is accurately documented before it ever reaches the billing stage. Understanding what CDI in healthcare is isn’t just about improving records; it’s about unlocking cleaner claims, faster reimbursements, and stronger revenue cycles.
With a well-structured healthcare CDI program, organizations can significantly reduce denials, enhance coding precision, and ensure every claim truly reflects the care delivered. If you’re serious about improving CDI in medical coding and want to know how a CDI specialist improves the accuracy of the claim being submitted, this guide will walk you through everything you need to know, clearly, practically, and with real impact.
Exploring Clinical Documentation Improvement (CDI)
CDI in healthcare (Clinical Documentation Improvement) is the process of ensuring that patient medical records are accurate, complete, and fully reflective of the care provided. It focuses on improving the quality of clinical documentation so that it supports correct coding, billing, and overall healthcare outcomes.
At its core, CDI acts as a bridge between clinical care and administrative processes. While physicians focus on treating patients, CDI ensures that every diagnosis, condition, and procedure is clearly documented in a way that supports compliance and reimbursement.
Why CDI is Critical in Healthcare:
- Ensures accurate representation of patient conditions
- Supports proper reimbursement and billing accuracy
- Reduces claim denials and audit risks
- Improves data quality for reporting and analytics
What Happens Without CDI?
Without a structured CDI process:
- Important diagnoses may be missed
- Claims may be undercoded or denied
- Healthcare organizations may lose significant revenue
In simple terms, if it’s not documented, it doesn’t exist, at least from a billing and compliance perspective.
How Do Healthcare CDI Programs Function?
A healthcare CDI program is a structured approach used by hospitals, clinics, and medical billing companies to improve documentation accuracy throughout the patient care journey.
It ensures that clinical documentation aligns with coding standards and payer requirements, ultimately leading to cleaner claims and faster reimbursements.
Step-by-Step Process of Healthcare CDI:
- Patient Encounter Documentation
Physicians document diagnoses, treatments, and procedures during patient care. - CDI Review (Concurrent or Retrospective)
CDI specialists review records in real-time or after discharge to identify gaps or inconsistencies. - Physician Queries
If documentation is unclear or incomplete, CDI specialists send queries to providers for clarification. - Documentation Enhancement
Providers update records to reflect accurate and specific patient conditions. - Final Coding & Billing
Coders assign appropriate codes based on improved documentation, ensuring compliant claims submission.
Key Elements of an Effective Healthcare CDI Program:
- Real-time (concurrent) documentation reviews
- Strong collaboration between providers and coders
- Standardized query processes
- Continuous education and training
A well-executed CDI program doesn’t just fix documentation; it transforms the entire revenue cycle.
The Impact of CDI on Coding Accuracy
CDI in medical coding plays a vital role in ensuring that the codes assigned to a patient’s record accurately reflect their condition, severity, and the care provided.
Medical coding relies entirely on documentation. If the documentation lacks detail, coders are forced to assign less specific codes, even if the patient’s condition was more complex.
How CDI Improves Medical Coding:
- Enhances coding specificity and accuracy
- Ensures proper assignment of ICD-10, CPT, and HCPCS codes
- Supports accurate DRG (Diagnosis-Related Group) classification
- Reduces coding errors and compliance risks
Real-World Example:
A physician documents “pneumonia,” but fails to specify the type or severity. With CDI intervention, the documentation may be clarified to “aspiration pneumonia with acute respiratory failure,” which:
- Reflects higher severity
- Justifies higher reimbursement
- Improves patient data accuracy
Why This Matters for Revenue:
Without CDI:
- Organizations risk undercoding and revenue loss
- Claims may not reflect the true complexity of care
- Audit risks increase
With CDI:
- Every claim tells the complete and accurate clinical story
- Coding becomes more precise
- Reimbursement aligns with actual services provided
The Role of a CDI Specialist in Healthcare
A CDI specialist is one of the most critical players in the healthcare revenue cycle. Their primary role is to ensure that clinical documentation is not only complete but also precise enough to support accurate coding and compliant claims submission.
They work at the intersection of clinical care, coding, and billing, making sure nothing gets lost in translation.
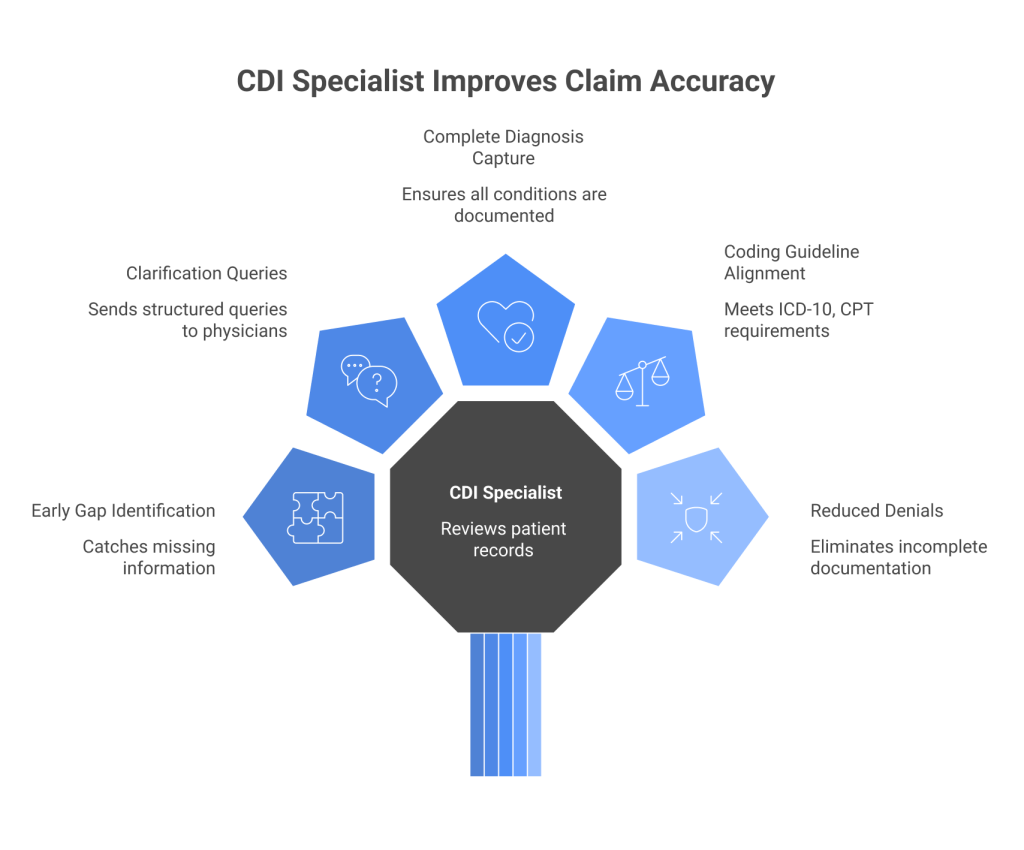
How a CDI Specialist Improves Claim Accuracy?
Identifies Documentation Gaps Early
CDI specialists review patient records to catch missing, vague, or inconsistent information before it impacts coding. This proactive approach prevents errors from reaching the billing stage.
Sends Queries for Clarification
When documentation is unclear, CDI specialists send structured queries to physicians to clarify diagnoses, severity, or procedures.
Example:
- “Sepsis” vs. “Severe sepsis with organ dysfunction.” This level of detail can significantly impact reimbursement and compliance.
Ensures Complete Capture of Diagnoses
They make sure all relevant conditions, comorbidities, and complications are documented properly.
This leads to:
- More accurate patient profiles
- Better risk adjustment
- Proper reimbursement
Aligns Documentation with Coding Guidelines
CDI specialists ensure that documentation meets ICD-10, CPT, and payer-specific requirements, making it easier for coders to assign the correct codes.
Reduces Claim Denials and Rework
Incomplete or unclear documentation is one of the biggest reasons for claim denials. CDI specialists eliminate this issue at the source.
The Real Business Impact
Organizations that invest in CDI specialists often experience:
- Fewer claim rejections
- Faster reimbursement cycles
- Increased revenue capture
- Stronger audit readiness
In short, CDI specialists don’t just improve documentation; they directly protect and grow your revenue.
Benefits of CDI in Healthcare Systems
Implementing CDI in healthcare isn’t just about compliance; it’s about creating a smarter, more efficient, and financially stable system.
Financial Benefits
- Improved reimbursement accuracy
- Reduced undercoding and missed charges
- Lower denial rates and rework costs
- Optimized revenue cycle performance
Clinical Benefits
- More accurate patient health records
- Better care coordination across teams
- Improved patient outcomes and safety
- Enhanced clinical decision-making
Operational Benefits
- Stronger compliance with regulations
- Better performance in audits
- Improved reporting and analytics
- Increased efficiency across departments
Competitive Advantage
Healthcare organizations with strong healthcare CDI programs outperform competitors by:
- Capturing the full value of services provided
- Maintaining cleaner claims
- Building trust with payers and regulators
Common Challenges in Healthcare CDI
Despite its benefits, implementing CDI in healthcare comes with challenges that can limit its effectiveness if not addressed properly.
Incomplete or Vague Physician Documentation
Physicians often work under time pressure, which can lead to:
- Missing details
- Non-specific diagnoses
- Inconsistent terminology
Lack of CDI Awareness and Training
Without proper training:
- Providers may not understand documentation requirements
- Coding and CDI teams may lack alignment
Communication Gaps Between Teams
A disconnect between:
- Physicians
- Coders
- CDI specialists
…can lead to delays, errors, and missed opportunities for clarification.
Time Constraints in Clinical Settings
Providers may not prioritize documentation improvement due to heavy workloads, leading to:
- Delayed responses to queries
- Incomplete records
How to Overcome These Challenges?
- Provide Continuous Training: Educate physicians and staff on documentation best practices.
- Implement Technology Solutions: Use CDI software and AI tools to streamline reviews and queries.
- Encourage Collaboration: Create a culture where CDI, coding, and clinical teams work together seamlessly.
- Standardize Processes: Develop clear guidelines for documentation and query handling.
How to Build a High-Performing CDI Program?
To fully leverage CDI in healthcare, organizations need more than just a process; they need a strategy. Implementing the right best practices ensures long-term success, improved documentation quality, and consistent financial outcomes.
Conduct Regular Documentation Audits
Frequent audits help identify gaps, trends, and areas for improvement in clinical documentation.
Why it matters:
- Detects recurring errors
- Improves coding accuracy over time
- Strengthens compliance
Train Physicians on Documentation Standards
Physicians play a central role in CDI success. Ongoing education ensures they understand the importance of detailed and specific documentation.
Focus areas:
- Specific diagnoses
- Severity and acuity
- Comorbidities and complications
Use Concurrent CDI Reviews
Reviewing documentation in real-time (during patient care) allows issues to be corrected immediately.
Benefits:
- Faster query resolution
- More accurate documentation
- Reduced retrospective corrections
Leverage Technology and AI Tools
Modern CDI solutions use automation and AI to flag documentation gaps and suggest improvements.
Results:
- Increased efficiency
- Reduced manual workload
- Better data accuracy
Track Key Performance Indicators (KPIs)
Monitor CDI performance using metrics such as:
- Query response rate
- Case mix index (CMI)
- Denial rates
- Coding accuracy
Foster Cross-Team Collaboration
Strong communication between CDI specialists, coders, and providers is essential.
Outcome:
- Faster workflows
- Fewer errors
- Better documentation quality
Summary
In today’s high-stakes healthcare environment, CDI in healthcare is not just a support function; it’s a strategic necessity. From improving medical coding accuracy to ensuring compliant and clean claims, CDI impacts every stage of the revenue cycle.
Organizations that truly understand what CDI is in healthcare and invest in strong healthcare CDI programs gain a clear advantage:
- Higher revenue capture
- Fewer denials
- Better compliance
- Improved patient data accuracy
More importantly, they position themselves for long-term success in an industry that demands precision, transparency, and accountability.
If your organization is still struggling with documentation gaps or claim inaccuracies, now is the time to act. Strengthening your CDI in medical coding processes and leveraging skilled CDI specialists can transform your revenue cycle from reactive to optimized.





