If you’re a Nurse Practitioner practicing in a Full Practice Authority (FPA) state, you’ve likely had this frustrating moment: your nurse practitioner credentialing application gets rejected, not because you did anything wrong, but because an insurance portal insists you list a supervising physician you legally don’t need.
You’re not alone. Across the country, independent NPs are running into outdated payer systems that haven’t caught up with modern laws, delaying approvals, disrupting cash flow, and creating unnecessary confusion.
The good news? This isn’t a legal problem; it’s a fixable administrative gap. In this guide, you’ll learn exactly how to navigate these rejections, complete independent NP enrollment successfully, and use a proven workaround to get your application approved, without compromising your autonomy.
What Full Practice Authority (FPA) Actually Means?
Full Practice Authority (FPA) allows Nurse Practitioners to evaluate patients, diagnose conditions, interpret diagnostic tests, and initiate treatment plans, including prescribing medications, without physician supervision or collaborative agreements. In FPA states, this independence isn’t optional; it’s legally recognized and protected.
This also means NPs are eligible for autonomous billing, allowing them to credential, enroll, and bill insurance payers under their own NPI. From a legal standpoint, there is no requirement to list a supervising physician because the role simply does not exist in your practice model.
Why Insurance Portals Still Require a Supervising Physician
Here’s where things get messy. Despite clear state laws, many payer enrollment systems still force you to enter a “collaborating” or “supervising” physician. Why?
- Legacy Software Systems: Many insurance portals were built before FPA laws expanded and haven’t been updated.
- Standardized National Templates: Payers often use uniform credentialing workflows across all states, ignoring local regulations.
- Risk-Averse Policies: Some payers maintain outdated requirements internally, even if they conflict with current laws.
The result? You’re asked to provide information that doesn’t apply to your practice, creating confusion and unnecessary rejections during the nurse practitioner credentialing process.
The Real Gap: State Law vs. Insurance Payer Policy
On paper, the law is clear: in FPA states, NPs practice independently. But in practice, insurance payers don’t always align with that reality. This creates a frustrating disconnect between payer policy and state law.
- State Law: Grants you full independence
- Payer Systems: Still assume physician oversight
This gap is the root cause of most independent NP enrollment issues. It’s not that you’re doing something wrong; it’s that the system hasn’t caught up.
Common Payer Rejection Scenarios
If you’ve gone through enrollment recently, these probably look familiar:
- “Supervising physician information missing.”
- “Collaborative agreement not provided.”
- Application flagged as incomplete due to blank required fields
- Automatic system rejection without manual review
These are not compliance failures; they’re system limitations. Recognizing this distinction is key because it shifts your strategy from “fixing your application” to working around outdated processes effectively.
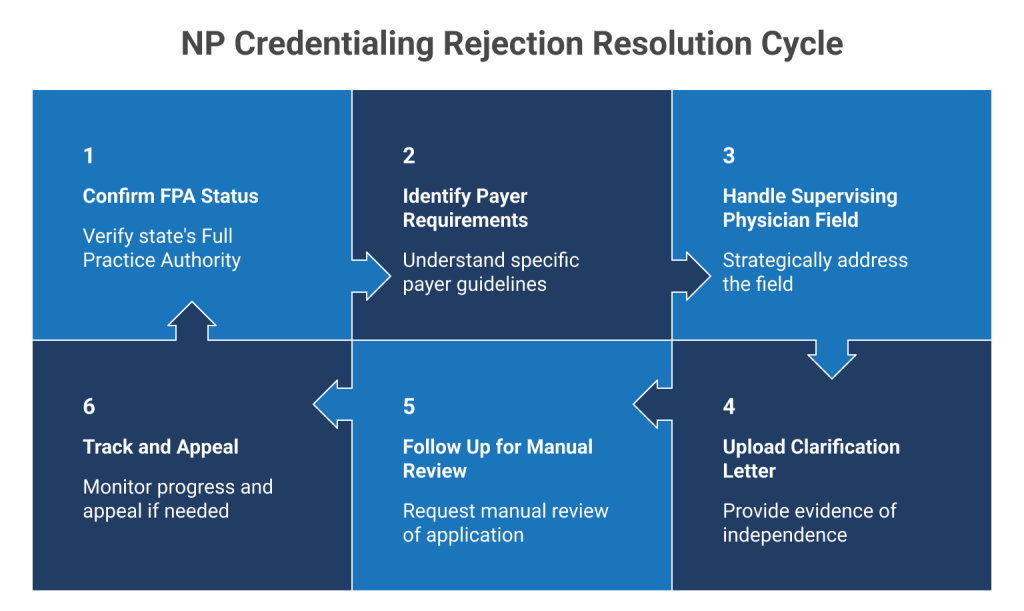
Step-by-Step: How to Fix NP Credentialing Rejections
This is where things turn in your favor. Once you understand that the issue is administrative, not legal, you can take specific, repeatable steps to bypass these roadblocks and complete your nurse practitioner credentialing successfully.
Step 1: Confirm Your State’s FPA Status
Before pushing back on a payer, make sure your state truly grants Full Practice Authority.
- Check your State Board of Nursing website
- Verify there are no collaboration or supervision requirements
- Save documentation or a screenshot for your records
This becomes critical evidence if you need to escalate your case.
Step 2: Identify Payer-Specific Requirements
Not all insurance payers behave the same way. Some are more updated than others.
- Review payer enrollment guidelines (if available)
- Contact provider enrollment or credentialing support
- Ask directly:
“How should independent NPs in FPA states complete the supervising physician section?”
Document every response. This gives you leverage if your application is rejected later.
Step 3: Handle the “Supervising Physician” Field Strategically
This is where most applications get stuck, but you have options:
- If the field is optional → Leave it blank
- If the system forces an entry →
- Enter “N/A – FPA State”
- Or use your own name (only if system validation requires a valid NPI format, use cautiously)
Avoid fabricating relationships. The goal is to stay compliant while navigating system limitations.
Step 4: Upload an “Independence Clarification Letter”
This is your strongest move, and where most NPs see success.
When the system doesn’t align with state law, you need to bridge the gap proactively.
- Upload the letter in:
- Supporting documents section
- Additional notes/upload fields
- Label it clearly:
“FPA Independence Clarification Required for Processing”
This immediately signals to reviewers that your application needs manual review, not auto-rejection.
Step 5: Follow Up and Push for Manual Review
Don’t just submit and wait.
- Call provider relations within 3–5 business days
- Reference your uploaded clarification letter
- Request manual override or review
Example phrasing:
“I’m an independent NP in an FPA state. My application may have been flagged due to system limitations. Can you confirm it’s being reviewed manually?”
Step 6: Track and Appeal if Necessary
If your application is still rejected:
- Request the specific reason in writing
- Submit a formal appeal referencing:
- State law
- Your independent status
- Your clarification letter
Persistence here often leads to approval, especially when you demonstrate compliance and clarity.
Tips to Avoid Future Credentialing Delays
Once you’ve successfully navigated one payer, the goal is to never deal with the same issue again. These best practices will streamline your nurse practitioner credentialing process and reduce friction across all future enrollments.
Maintain a Credentialing Packet:
Keep a ready-to-go folder with your license, DEA (if applicable), NPI confirmation, malpractice insurance, and your Independence Clarification Letter.
Standardize Your Responses:
Use consistent language across all applications when addressing supervision fields (e.g., “Independent NP – FPA State”).
Track Payer Behavior:
Create a simple spreadsheet noting which payers:
- Accept independent enrollment easily
- Require manual review
- Frequently reject applications
Submit Early & Follow Up Often:
Don’t wait for rejections; follow up proactively within a few days of submission.
Consider Credentialing Support Services:
If you’re scaling your practice, outsourcing parts of your independent NP enrollment process can save time and reduce errors.
These small systems can dramatically reduce delays and keep your revenue cycle running smoothly.
When Should You Escalate the Issue?
Sometimes, even after doing everything right, the system or the payer doesn’t cooperate. That’s when escalation becomes necessary.
Contacting Provider Relations
Start here before jumping to formal appeals.
- Call the payer’s provider enrollment or relations department
- Clearly state:
“I am an NP practicing independently in an FPA state, and my application appears to be incorrectly flagged.” - Ask for:
- Manual review
- Clarification on internal policy
Many issues are resolved at this stage once a human reviews your case.
Filing a Formal Appeal
If your application is denied:
- Request the denial reason in writing
Submit a structured appeal including:
- Your original application
- Independence Clarification Letter
- Supporting state law references
💡 Keep your tone professional and factual; this increases approval chances.
Referencing State Law in Appeals
This is your strongest leverage point.
- Cite your state’s Full Practice Authority (FPA) statute
Emphasize:
- No legal requirement for physician collaboration
- Your eligibility for NP autonomous billing
This shifts the conversation from “system requirement” to legal compliance, which payers take seriously.
Conclusion
The “collaborative physician” requirement in FPA states isn’t real; it’s a ghost created by outdated systems and policies. And while it can slow down your nurse practitioner credentialing, it doesn’t have to stop you.
By understanding the gap between payer policy vs. state law, using strategic workarounds, and advocating for your independent status, you can take full control of your independent NP enrollment, without compromising your autonomy.
You don’t need to change your practice to fit the system; you just need to know how to navigate it.
FAQs
Q: Do nurse practitioners need a collaborating physician in FPA states?
Ans: No. In Full Practice Authority states, NPs are legally allowed to practice independently without physician supervision or collaboration.
Q: Why is my independent NP enrollment being rejected?
Ans: Most rejections happen due to outdated payer systems that still require supervising physician details, even when state law does not.
Q: Can NPs bill independently in FPA states?
Ans: Yes. NPs can engage in autonomous billing using their own NPI, as long as they are properly credentialed with the payer.
Q: How do I fix nurse practitioner credentialing issues quickly?
Ans: The most effective approach is to:
- Submit your application correctly
- Upload an Independence Clarification Letter
- Follow up for manual review
Q: What if the payer refuses to accept my independent status?
Ans: You can escalate by:
- Contacting provider relations
- Filing an appeal
- Referencing state law to support your case





